Eye Condition
Lattice Degeneration
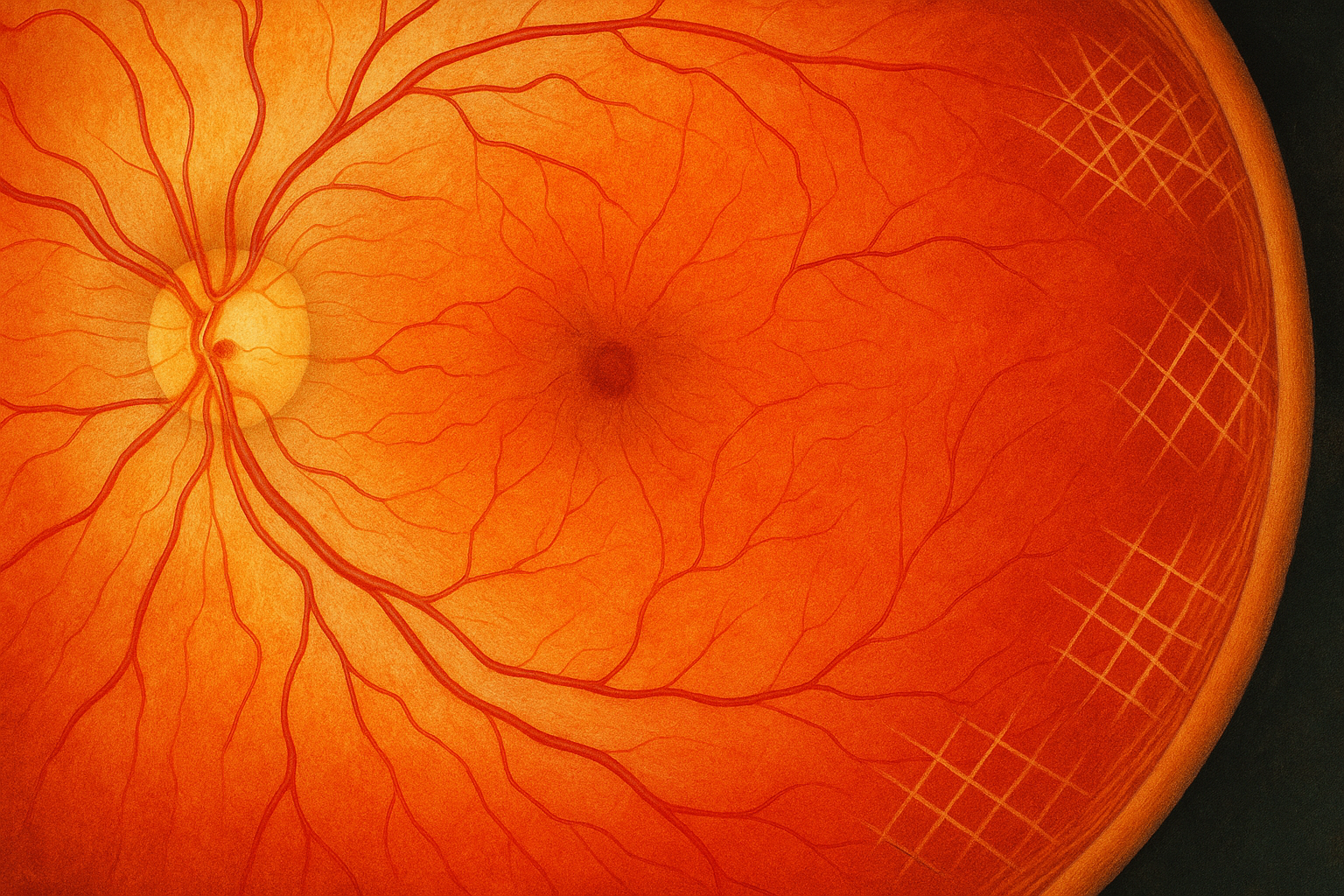
Lattice degeneration is thinning of the retina’s outer edge marked by crisscross white lines; usually symptom-free but can create holes or tears that raise detachment risk.
Explore our treatment options for Lattice Degeneration
What is Lattice Degeneration?
Lattice degeneration is a peripheral retinal condition in which patches of tissue become thin, shrunken, and crisscrossed by fine white lines. These lines create the “lattice” pattern an eye doctor sees during a dilated exam. The affected zones lie well outside the macula, so central vision usually stays sharp. Roughly 7 – 8 percent of people have lattice degeneration, and almost half of them develop it in both eyes. Because the weakened areas are symptom-free, most people learn they have lattice degeneration only after a routine check-up. While many lesions remain stable for life, a small percentage can progress to retinal holes or tears that may lead to a detachment if left unaddressed.
Key symptoms and early warning signs
Patients usually feel nothing from uncomplicated lattice degeneration, but warning signs can appear if a break develops nearby. Watch for:
- Sudden shower of new floaters, especially dark specks or “cobwebs”
- Flashes of light at the edge of vision
- A gray curtain or shadow drifting across side vision
- Sudden loss of side vision or central blur
If you notice any of these symptoms, arrange an urgent eye evaluation right away.
How Lattice Degeneration is diagnosed
An eye doctor can identify lattice degeneration during a dilated retinal examination with bright binocular lenses or ultra-widefield imaging. Key studies include:
- Dilated fundus examination to inspect the peripheral retina under high magnification
- Optical coherence tomography (OCT) for cross-sectional views of suspicious areas
- Fundus photography or widefield scanning laser images to document lesion size and location
- B-scan ultrasound if media are cloudy or a detachment is suspected
These tests help map lesions, look for tiny holes, and determine whether preventive treatment is advisable.
Why it happens: causes and risk factors
Scientists do not know the exact trigger, but several factors appear to thin and crease the retina’s edge:
- Nearsightedness (myopia)—lattice affects up to one-third of highly myopic eyes
- Aging and natural vitreous liquefaction after the twenties
- Family history of peripheral retinal thinning
- Previous eye trauma or surgery that alters vitreous support
- Systemic collagen disorders that weaken connective tissue
Race and sex do not meaningfully change risk. Because retinal tissue is already thinner in myopic eyes, any extra thinning can produce atrophic holes within a lattice patch.
Conventional treatment options
Most lattice lesions never need intervention. Standard care focuses on:
- Observation with yearly or semi-annual dilated exams
- Barrier laser photocoagulation around fresh holes or symptomatic tears to “weld” retina in place
- Cryotherapy in select cases where laser cannot reach
- Pars plana vitrectomy and scleral buckle only if a full retinal detachment occurs
Preventive laser is controversial; ophthalmologists weigh patient age, myopia degree, lesion size, and symptoms before deciding.
Eye Health Institute’s integrative approach
At the Eye Health Institute, we view lattice degeneration as a signal to strengthen the entire retinal environment—not only to monitor weak spots. Dr. Andy Rosenfarb and the team combine evidence-informed therapies designed to promote circulation, metabolic resilience, and tissue repair:
-
Micro Acupuncture 48 and electro-acupuncture
Precisely placed needles and gentle electrical current aim to stimulate ocular blood flow and neurotrophic signaling, supporting retinal cell health. -
Microcurrent stimulation (ACS-3000 device)
Low-level currents, delivered in-clinic or through a home program, may encourage mitochondrial activity and aid fluid exchange. -
Targeted herbal and nutritional support
We customize antioxidants (lutein, zeaxanthin), omega-3 fatty acids, and botanicals that modulate inflammation and oxidative stress—two drivers of retinal thinning. -
Hydrogen therapy and hyperbaric oxygen options
When appropriate, these modalities can reduce reactive oxygen species and improve tissue oxygenation. -
Lifestyle and stress management coaching
Adequate sleep, blood sugar control, and eye-safe movement habits (protective eyewear for sports) help lower the chance of a retinal tear.
Programs begin with a comprehensive retinal imaging session, followed by an intensive treatment block or a blended in-office/at-home plan. Progress is tracked with OCT and widefield scans to confirm stability. While no therapy can “re-grow” lost retinal tissue, our integrative care may help reinforce vulnerable zones and preserve peripheral function alongside standard ophthalmic monitoring.
What patients report / clinical insights
Many patients tell us that learning they have lattice degeneration feels unsettling because it is invisible day-to-day. Clear imaging reviews and a concrete wellness plan provide reassurance. After several weeks of combined acupuncture and microcurrent sessions, some clients note crisper side vision and fewer night floaters. Objective scans often show unchanged lesion borders, suggesting stability. The biggest win, however, is confidence: patients understand which symptoms require an emergency call, which activities are safe, and how diet, supplements, and stress reduction may support long-term retinal vitality.

When to seek urgent care
Get urgent eye care for sudden vision loss, a gray curtain over vision, many new floaters with flashes, severe eye pain, or eye trauma. These can signal a retinal tear or detachment that requires immediate treatment to protect sight. If you experience any rapid change in vision, call your ophthalmologist or go to the nearest emergency eye clinic without delay. Early intervention can be sight-saving.